Concerns grow worldwide as rare Monkeypox virus spreads like wildfire: Virologists ‘can not explain’ speed and scale
Virologists around the world are increasingly sounding the alarm bell over the rapid spread of the rare Monkeypox virus, which is usually found in parts of Western Africa.
The confirmed number of cases climbed to 80 over the weekend, in 12 countries around the world, including the UK, Belgium, France, Netherlands and Australia.
The well-respected Belgian virologist Marc van Ranst, of Leuven University, said that most of his colleagues around the world are ‘taken by surprise’ by the scale and speed the virus seems to be spreading.
“This outbreak, in multiple continents, in multiple countries, is taking us by surprise. We cannot explain this.”
Marc van Ranst,
Van Ranst stressed “This is a very rare situation, we usually only see one or two cases pop up outside Africa, and onkly once in a while,” Van Ranst told Dutch news program Nieuwsuur.
Monkeypox is a viral infection usually associated with travel to West Africa.
It is usually a mild self-limiting illness, spread by very close contact with someone with monkeypox and most people recover within a few weeks.
‘Unusual’
Professor Sir Peter Horby, director of the Pandemic Sciences Institute at Oxford University, has described the current monkeypox outbreak as “an unusual situation”, because the virus is being transmitted within communities outside of Central and West Africa.
Sir Peter told BBC Radio 4’s Today programme: “It’s transmitted by close person-to-person contact and, in the past, we have not seen it being very infectious.
“What’s unusual about what we’re seeing now is that we’re seeing transmission occurring in the community in Europe and now in other countries, so it’s an unusual situation where we seem to have had the virus introduced but now have ongoing transmission within certain communities.”
Sir Peter added: “It would appear that there is some element of sexual transmission perhaps with just the very close contact between people and the skin lesions, because a large proportion of the current cases are being detected in gay and bisexual men.
“It is very important that we get the message across that if people have unusual skin lesions that they do seek attention quickly so that we can control this.”
Professor Sir Peter Horby.
“The important thing is that we interrupt transmission and this doesn’t become established in the human population in Europe.”
Another 11 people in Britain have been confirmed to have monkeypox, bringing the total number of cases of the virus up to 20. There are confirmed cases in nine countries outside of Central and West Africa.
Symptoms
Initial symptoms of monkeypox include fever, headache, muscle aches, backache, swollen lymph nodes, chills and exhaustion.
The virus spreads through close contact and UKHSA is advising individuals, particularly those who are gay, bisexual or MSM, to be alert to any unusual rashes or lesions on any part of their body, especially their genitalia, and to contact a sexual health service if they have concerns.
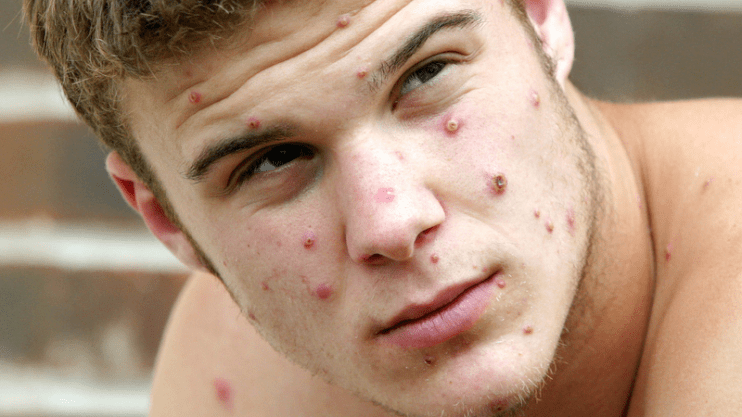
A rash can develop, often beginning on the face, then spreading to other parts of the body including the genitals.
The rash changes and goes through different stages, and can look like chickenpox or syphilis, before finally forming a scab, which later falls off.
Contact during sex
Monkeypox has not previously been described as a sexually transmitted infection, though it can be passed on by direct contact during sex.
It can also be passed on through other close contact with a person who has monkeypox or contact with clothing or linens used by a person who has monkeypox.

A top doctor warned this weekend that Monkeypox could have a “massive impact” on access to sexual health services.
The disease, which was first found in monkeys, can be transmitted from person to person through close physical contact – including sexual intercourse – and is caused by the monkeypox virus.
The number of cases confirmed in Britain has hit 20 with nine other countries outside of Central and West Africa also reporting outbreaks.
Dr Claire Dewsnap, president of the British Association for Sexual Health and HIV, said she is concerned about how the infection could affect services because staff who come in contact with sufferers are forced to isolate.
She told the BBC that clinic staff were “already under significant pressure” before monkeypox was identified, making the situation worse.
“It is already stretching the workforce and will have a massive impact if staff have to isolate if they are in close contact with someone who’s infected,” Dr Dewsnap said.
“In terms of the infection and its consequences for individuals, I’m not that concerned,” she later told BBC Radio 4.
“I am concerned about our ability to maintain good sexual health services and access for everyone while still managing this new infection.”
Dr Claire Dewsnap, president of the British Association for Sexual Health and HIV
Dr Dewsnap also called for “adequate funding” for sexual health services.
She told BBC Breakfast: “Over the last 10 years, there’s been a significant decrease in funding through the public health budget.
“And that has seen a direct effect on staffing level and that means we have less capacity to see people.
“We used to be able to see people within 48 hours of them contacting us – that’s really important because it cuts down the window where people have an infection, they don’t know they have an infection and therefore they can pass it on to the people.
“So the speed in which we see people is really critical and monkeypox coming along shows us that more than ever before.
“So we need adequate funding so we can adequately staff with the experts that we need and the appropriately trained staff in clinics so that we can ensure people can get in quickly, and therefore we can reduce the risk of infection of other people.”