
How cutting-edge technology is helping curb the rise in avoidable blindness worldwide
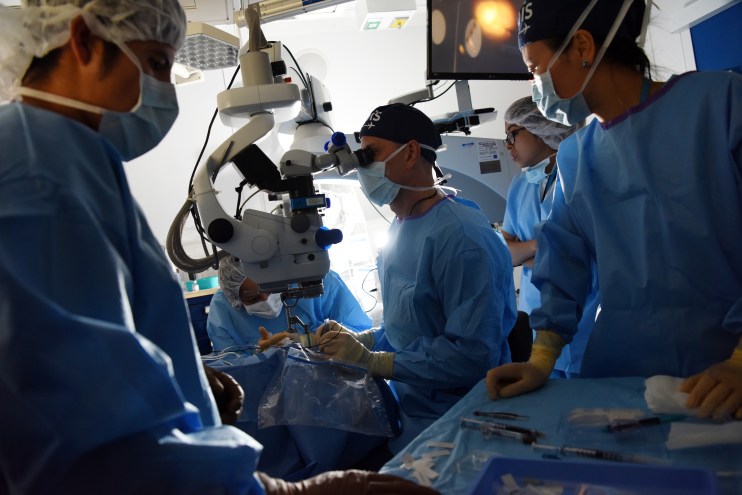
Globally 1.1 billion people live with vision loss and blindness and a shocking 90% of it is avoidable. Sadly, 9 out of 10 of these people live in low-to-middle-income countries with little or no access to eye health care. Orbis, an international sight-loss charity, works to fight avoidable blindness in these regions through hospital-based programmes and on board the Orbis Flying Eye Hospital – a cargo plane with a state-of-the-art operating theatre, recovery room and classroom.
Our teams of leading medical experts, including volunteer ophthalmologists, nurses and anaesthetists in the NHS, train the next generation of ophthalmic experts and eye healthcare workers across Africa, Asia, Latin America and the Caribbean. While also treating those living months, sometimes, years without basic eye care with sight-saving surgeries and medicines.

Living with avoidable blindness plunges communities and families into poverty as adults lose their livelihoods and children miss out on an education. And the numbers are rising. A further 60 million people are expected to be living with avoidable blindness by 2050.
Changes to our lifestyles, growing populations and people living for longer are all contributing to a rise in conditions such as diabetic retinopathy and myopia (near-sightedness).
With the global cost of living crisis causing a squeeze amongst households, communities and Government budgets, tackling the rise of avoidable blindness worldwide may seem like an impossible task and one we cannot afford to invest in.
But cutting-edge ophthalmic technology is one-way Orbis have helped to slow the rise on global blindness in recent years. Back in 2017, experts had in fact predicted global blindness would triple by 2050, but that figure has slowed – thanks to the efforts of organisations like Orbis and our partners.
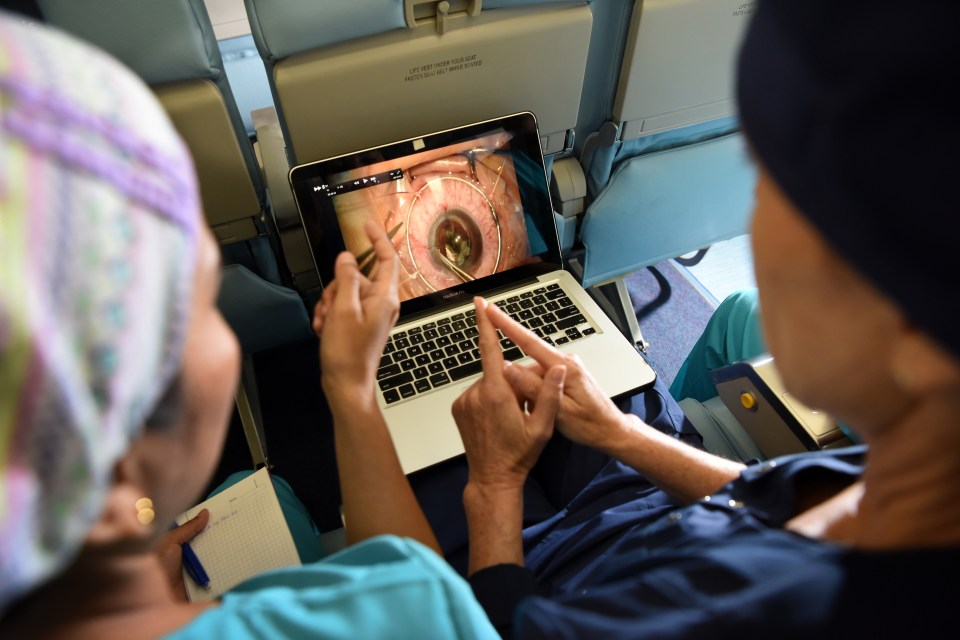
Technology is helping us to reach more people around the world.
On board the Orbis Flying Eye Hospital, a state-of-the-art mobile simulation centre including virtual reality, artificial eyes, and life-like mannequins, allows eye care professionals, wherever they are, to practice complex eye procedures safely until they are ready to perform surgery on people.
And our telemedicine platform Cybersight, ensures medical experts in remote regions can access on-the-spot consultations, live and interactive webinars and online training. While surgical mentorship ensures our team of ophthalmic experts can guide sight-saving surgery in real-time from half-way around the world.By the end of September 2022, Cybersight had 72,00 registered users in over 200 countries.
One such clinician whose work has been changed because of Cybersight is Tran Thi Hai, a first-year resident at Hanoi Medical University in Vietnam and winner of a prestigious Cybersight programme award. She said:
What’s amazing is that everything I questioned is on Cybersight. They know how to synthesize all sources of knowledge in such a comprehensible way, which helps me access lessons easily. Not to mention, Cybersight also has so many detailed videos and clear images of eye examinations and surgeries. When I learn from books, I would have to look for qualified examples myself, so Cybersight does save me lots of time.
When asked about which lessons are the most helpful, Hai said:
Videos like cataract surgeries are what interest me the most. I did have the chance to observe surgeries in real life, but the videos on Cybersight also provide comments of doctors during surgeries. I find that very easy to understand.”
What’s more, the impact on patients can be life-transforming. For patients who travel a great distance to have their exam, quick results can make all the difference in whether they get follow-up care.
Just some of those our teams have helped include Anika, 14, from a rural community in Bangladesh. She received glasses to correct her myopia (short-sightedness) thanks to a diagnosis from a doctor at a distant hospital made possible by telemedicine. She is now able to study once again. And Cuthbert from Barbados, who will see his three grandchildren again because his surgeon, Dr. Dawn Grosvenor, grew her skills with mentors from another continent.

With the need for trained ophthalmologists already outpacing the numbers that are trained, Cybersight and Orbis’ use of cutting-edge technology is helping to keep a generation of eye care professionals from falling behind in their education. While are also giving essential treatment to people like Anika and Cuthbert so they can hope for a better future.
We are working to make eye care available everywhere, for everyone, so no one has to experience the consequences of avoidable blindness. And we will continue to train more people in places than ever before, but we cannot do it alone.
To support our work and find out more about Orbis, visit www.orbis.org.uk