Prevention is the last chance left to save the NHS from an inevitable death spiral
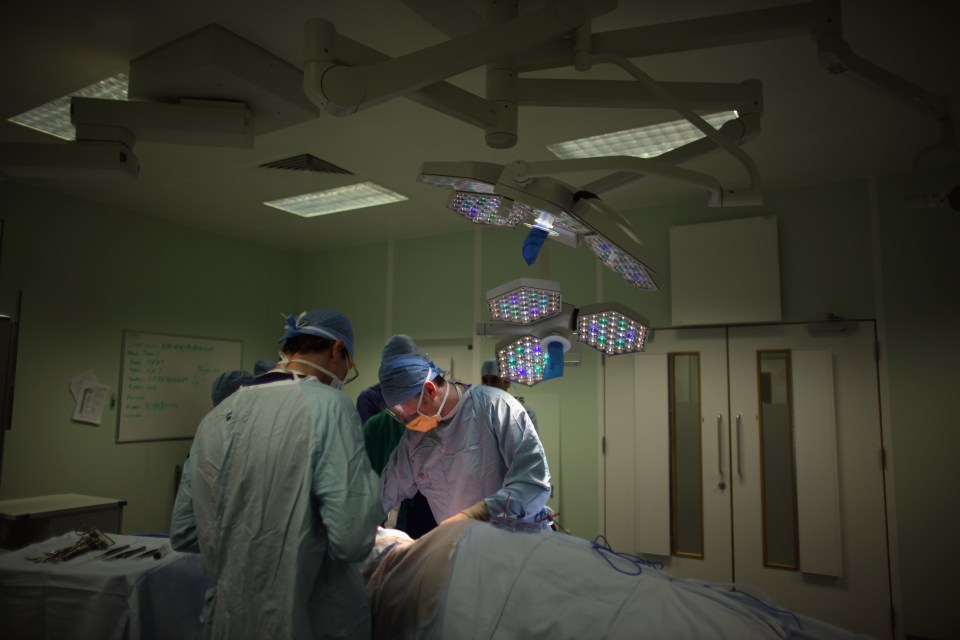
As NHS waiting lists reach a record high, we should seriously invest into prevention – so we can save lives, free up hospital beds and ultimately save money for the health service, writes Hamish Grierson
Late last week, the number of people waiting to start hospital treatment in England officially reached a record high. Cutting waiting lists is one of Rishi Sunak’s “five pledges” – and he clearly couldn’t be further from fulfilling it, with 10,737 people waiting more than 18 months to start treatment.
We know by now there is no silver bullet solution for the NHS crisis. But we’re not only failing to put out the fires in front of us; we’re also locking ourselves into decades more pain by failing to invest in the future.
Prevention is the best tool we have to address this health emergency. It means spotting the warning signs of disease early, helping to triage healthcare demand and reducing pressure on stretched services.
Take diabetes. It leads to more than 770 strokes and 590 heart attacks each week, but is largely preventable with the right diagnostics, monitoring, and self-management.
Self-monitoring of blood glucose – whereby people with diabetes measure their blood sugar themselves – has been demonstrated to improve HbA1c, your average blood sugar over the last three months.
A randomised control trial showed that a reduction of just 0.92 per cent of this blood sugar in insulin-treated type 2 diabetes patients was associated with a 2.3 per cent decreased 10-year risk for a fatal heart attack. This, in combination with a 10 per cent reduction of low blood sugar incidents, led to cost savings of around £4.5m a year for type-2 diabetics.
Many of the solutions are already at our fingertips, from lab capacity to diagnostics infrastructure. On top of that, we’re becoming an increasingly health literate population. It’s partially a positive legacy from the pandemic, where collaboration knocked down the walls between the public and private sectors.
So many of the rehashed arguments about the private sector and technology in healthcare miss the point. We already have a system where the richest can pay for self-funded medical procedures and health interventions. The question we need to be asking is why shouldn’t everyone have access to this care?
The NHS already commissions a whole host of companies to deliver services on its behalf. But we’re not focusing enough on the technology that can deliver the best return on investment in terms of preventing chronic disease.
Improving screening and prevention amongst people at risk of cardiovascular disease by as little as 10 per cent could help prevent 7 per cent of cardiovascular events, saving £2.4bn a year. Screening an additional 20 million people using at-home cholesterol panel tests would cost £200m, saving billions in the process. Home-run tests also ensure we’re able to target the people in the higher risk demographics, generally linked to a lower socio-economic status and to less accessibility to healthcare clinics or centres.
Redistributing spending to focus on preventive healthcare would ultimately reduce pressure on the NHS and its hospitals and save us money, paying for itself. Imagine getting the results of diagnostic tests on our phones, followed up by personalised information and advice about how to make relevant lifestyle changes to improve our health. A part of this is also equipping people with information of where to go – pharmacists play an important role here, not just GPs – if something acute requires attention.
Personalised data-driven insights are the basis of pretty much every service we engage with; it’s striking they’re not at the basis of health services too. Working on prevention would have a positive ripple effect throughout the whole NHS ecosystem, making life easier for overworked doctors and GPs, and ultimately freeing up space in hospitals for people who need to be seen. It’s a path forward we must seriously try.
