If your doctor can’t prescribe you antibiotics, watching and waiting will be the only alternative
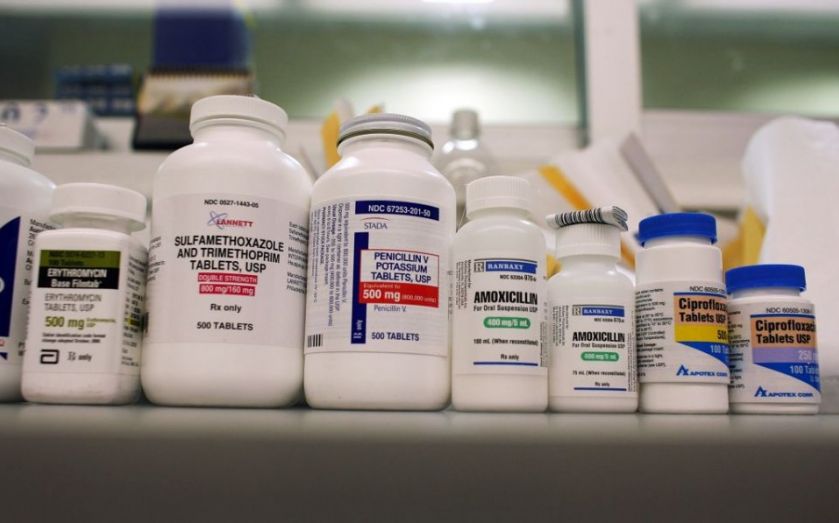
From now on, we'll have to endure our sore throats and sniffles for as long as they choose to plague us – doctors in the UK have been advised against prescribing antibiotics as readily as they do at the moment, which means people with minor ailments will just have to sit back and wait for the worst to be over.
Read more: The rising threat of antibiotic resistance: 80,000 could die from blood infection in the UK
The National Institute for Health and Care Excellence (Nice), the government's medical advisory body, warned today of the growing threat of antibiotic resistance – the more we use the limited range of antibiotics currently available, the more resistant they will grow to the micro-organisms they are trying to kill off.
“The more we use antibiotics, the less effective they become. Infections can evolve and become resistant to existing medicines” said Dr Tessa Lewis, GP and medical advisor to All Wales Medical Strategy Group.
We've already seen examples of this – the MRSA bacteria found in some hospitals in the UK is resistant to a number of widely used antibiotics, making it more difficult to treat than other bacterial infections.
Yet figures show that despite the risk, antibiotic prescribing has been steadily increasing in recent years, with 41.6m prescriptions having been handed out in 2013-2014 alone.
The danger is that if antibiotics continue to be handed out in high numbers, one day we'll revert back into the dark ages when bacterial diseases most of us haven't even heard of were major causes of death.
What's the alternative?
The dangers associated with antibiotic over-use are clear, but what does this mean for the sick people heading to the doctor in hope of getting their hands on a cure?
According to Nice's guidance, it will mean that unless a person has a serious health problem that requires urgent use of antibiotics, they'll be required to wait and see if the infection clears up on its own, without medical intervention.
One way of putting this into action would be via delayed prescribing, where the patient is given a prescription for the antibiotic only if there has been no improvement after a period of waiting.
Mark Baker, director of the centre for clinical practice at Nice, said:
The guideline recommends that prescribers take time to discuss with patients the likely nature of their condition, the benefits and harms of immediate antimicrobial prescribing, alternative options such as watchful waiting and/or delayed prescribing and why prescribing an antimicrobial may not be the best option for them – for example, if they have a self-limiting respiratory tract infection.The guideline also recommends that patients are given advice about who they should contact if they have concerns about infection after discharge from hospital.