Drug shortages hitting UK patient care more than anywhere else in Europe

Medicines shortages are hitting patient care in the UK and across Europe, according to a report published by the European Association of Hospital Pharmacists (EAHP).
The UK's healthcare system fared especially badly in the report compared with its continental neighbours, with 100 per cent of the hospital pharmacists from the UK saying they "strongly agreed" with the statement “medicines shortages in my hospital are having a negative impact on patient care”.
UK pharmacists added that they had to devote up to 10 hours a week to managing the problem of shortages.
The only country to come even remotely close to the UK's level of pessimism was Malta, where 66.6 per cent agreed with the statement. The UK's healthcare system was a far cry from Switzerland and Denmark where a little over 10 per cent agreed.
The consequences for some patients could be dire with some patients suffering deterioration in their condition or having or postponements in their treatment.
A hospital pharmacist from Staffordshire commented in the report:
A shortage of KwellsTM [hyoscine] has meant our clozapine [used for schizophrenia] patients are suffering from hypersalivation
[excessive salivation, known side effect of clozapine] unnecessarily.
Another pharmacist from Cheshire added:
Teicoplanin [antibiotic] shortage prompted review and change of antibiotics for many patients in our hospital. These alternative agents had a higher association with clostridium difficile and was not the optimum choice for patients.
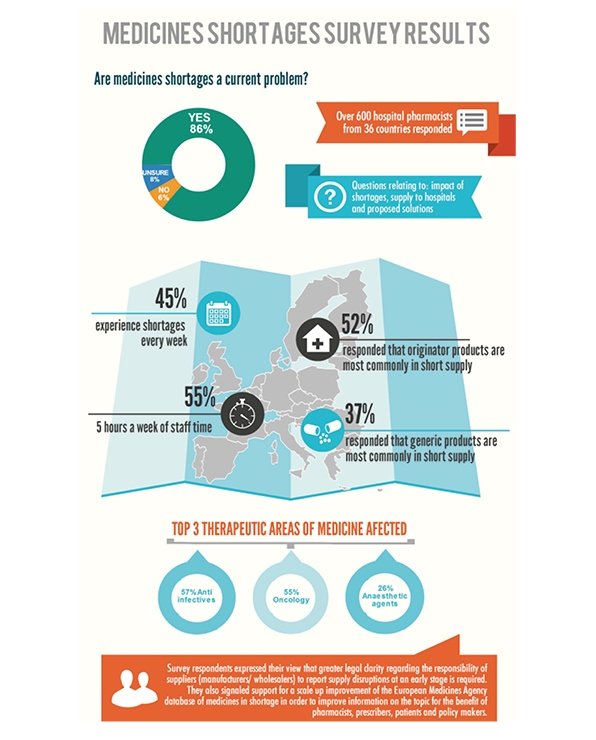
The report surveyed 600 hospital pharmacists in 36 European countries. The UK was far from alone in suffering problems with a lack of vital drugs. Across the continent, 66 per cent of participants said they experienced medicines shortages as a daily or weekly problem.
A Maltese pharmacist commented on the problems encountered at some NHS pharmacies:
Patients who get their out-patient treatment from an NHS pharmacy sometimes require hospital admission because they are not available.
The EAHP produced a video to accompany the report: